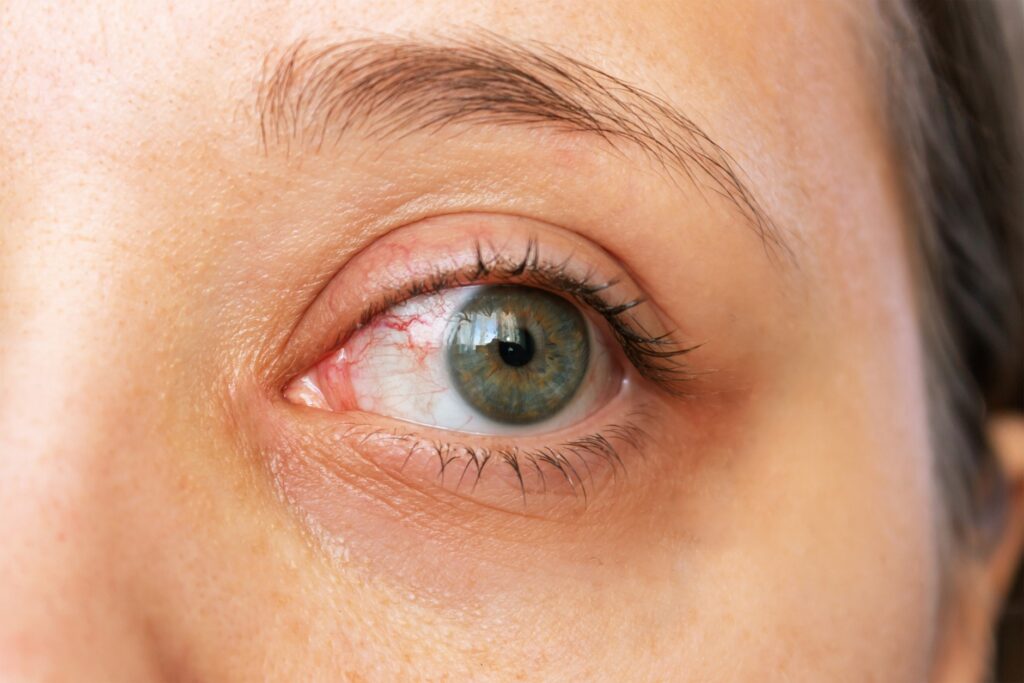
Uveitis is a serious eye condition that impacts the uvea, which is the middle layer of the eye, consisting of the iris, ciliary body, and choroid.
This condition can cause pain, blurred vision, redness and if left untreated, can lead to severe complications such as vision loss. Uveitis is not just one disease; it’s an umbrella term that encompasses a variety of conditions that affect the uvea. Whether it’s acute or chronic, mild or severe, early diagnosis and treatment are essential for managing uveitis and preventing long-term damage.
What is Uveitis?
Uveitis refers to the inflammation of the uvea, which provides nutrients to the retina. The uvea is composed of three main sections: the iris (colored part of the eye), the ciliary body (which controls the lens’s shape), and the choroid (blood vessels that nourish the retina). Inflammation in this area can affect one or more of these components, leading to varying degrees of discomfort and visual impairment.
There are four main types of uveitis based on the affected area of the eye:
- Anterior Uveitis: Affects the front of the eye, particularly the iris.
- Intermediate Uveitis: Involves the ciliary body and the vitreous humor.
- Posterior Uveitis: Inflammation of the choroid and retina.
- Panuveitis: Involves inflammation in all layers of the uvea.
Symptoms of Uveitis
Uveitis often comes on suddenly and may lead to a range of symptoms that can vary depending on the type and severity of the inflammation. Some common symptoms include:
- Eye redness: The most obvious sign of uveitis is caused by blood vessels inflammation in the eye.
- Eye pain: Often described as a deep, aching pain that may worsen with light.
- Blurred vision: Vision may become cloudy or dim due to swelling and inflammation affecting the retina or other parts of the eye.
- Sensitivity to light (photophobia): Light may become unbearably bright, causing discomfort or pain.
- Tearing: Excessive watering of the eyes is common in some cases.
- Floaters: Dark spots or specks that float across your field of vision.
If you experience any of these symptoms, it is essential to seek medical attention immediately. Untreated uveitis can lead to more severe complications such as glaucoma, cataracts, retinal damage, or even permanent vision loss.
Causes of Uveitis
The exact cause of uveitis can vary and is not always clear. In many cases, the condition is associated with underlying diseases, infections, or autoimmune disorders. Some of the most common causes include:
- Autoimmune Diseases: Conditions like rheumatoid arthritis, lupus, and ankylosing spondylitis can trigger the body’s immune system to attack its own tissues, leading to inflammation in the uvea.
- Infections: Certain infections, such as tuberculosis, herpes simplex, and syphilis, can lead to uveitis. Infections can directly affect the eye or cause inflammation as a secondary effect.
- Trauma: Injury to the eye can lead to uveitis, especially if it involves penetration of the eyeball.
- Surgery: Eye surgeries, including cataract surgeries, can occasionally lead to uveitis.
- Genetic Factors: Some individuals may have a genetic predisposition that makes them more susceptible to developing uveitis.
- Other conditions: Inflammatory conditions such as Crohn’s disease or sarcoidosis can also be linked to uveitis.
In some cases, no underlying cause is identified, and the condition is referred to as “idiopathic” uveitis.
Diagnosis of Uveitis
Diagnosing uveitis involves a thorough eye examination by an ophthalmologist. Several diagnostic tests may be required to determine the cause and extent of the inflammation. These may include:
- Slit-lamp examination: This allows the doctor to closely examine the structures of the eye under high magnification and identify any signs of inflammation.
- Fundus examination: This test involves looking at the back of the eye (the retina and choroid) to check for any signs of damage or inflammation.
- Blood tests: Blood work can help determine if there is an underlying infection or autoimmune condition causing the uveitis.
- Imaging tests: If needed, imaging techniques such as optical coherence tomography (OCT) or fluorescein angiography may be used to visualize the retina and identify abnormalities.
Early diagnosis is crucial for effective treatment and prevention of long-term damage to the eye.
Treatment Options for Uveitis
The goal of treatment is to reduce inflammation, relieve symptoms, and prevent complications. The type of treatment used depends on the severity and cause of the uveitis. Common treatment options include:
- Medications
- Corticosteroids: These are the most commonly used medications for uveitis. They help to reduce inflammation and are typically administered as eye drops, oral tablets, or injections around the eye.
- Immunosuppressive drugs: If the uveitis is caused by an autoimmune disorder, medications that suppress the immune system, such as methotrexate or azathioprine, may be prescribed.
- Antibiotics or antiviral drugs: If an infection is the cause of uveitis, antibiotics or antiviral medications will be used to treat the infection.
- Surgery
In some cases, especially when complications such as cataracts or glaucoma occur, surgery may be necessary. Surgical procedures may include:
- Cataract removal: In cases where a cataract develops as a result of uveitis, surgery to remove the cataract may be needed.
- Glaucoma surgery: If uveitis leads to high intraocular pressure (glaucoma), surgery may be required to correct this.
- Vitrectomy: In rare cases, surgery to remove the vitreous gel from the eye may be performed to treat severe inflammation or damage to the retina.
- Lifestyle and Home Care
- Regular follow-up: Continuous monitoring of eye health is essential in managing uveitis.
- Rest: Adequate rest can help the body heal and manage symptoms.
- Protective eyewear: Sunglasses or special eye shields can help reduce light sensitivity and protect the eyes.
Preventing Uveitis Complications
With prompt treatment and proper management, many individuals with uveitis can prevent long-term damage to their vision. However, uveitis can recur, and it’s important to follow your doctor’s instructions to minimize the risk of flare-ups. Regular eye exams are essential for early detection of complications.
Living with Uveitis
Uveitis can be a chronic condition, and its impact on vision can affect a person’s quality of life. However, with proper care and lifestyle adjustments, many people can lead fulfilling lives while managing the condition. Understanding the signs of an impending flare-up and seeking immediate care can help minimize the long-term effects.
Conclusion: Protect Your Vision, Seek Help Early
Uveitis is a serious eye condition that requires timely diagnosis and treatment. If you experience symptoms like eye pain, redness, blurred vision, or light sensitivity, it’s important to consult an ophthalmologist right away. Early intervention can help prevent permanent vision damage and improve your quality of life.
Take charge of your eye health today. Schedule a consultation and protect your vision!